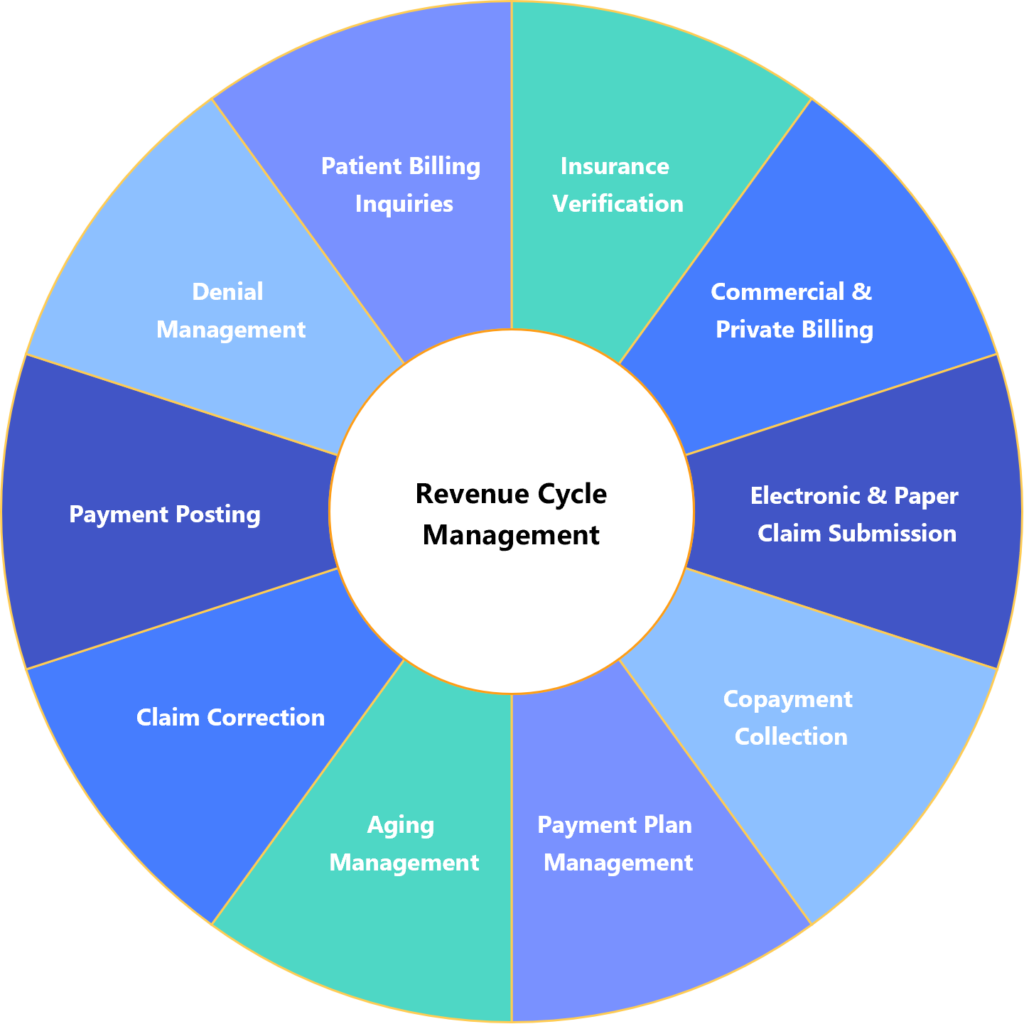
Insurance Verification: Verify patient eligibility and benefits with insurance providers, document details in the client’s EHR, and communicate updates to the client and/or patient.
Claims Management & Billing
Submit claims to commercial insurers and private payers, ensure accurate balances, and flag any discrepancies for review.
Claim Submission (Electronic & Paper) Prepare and submit all claims promptly to ensure timely reimbursement.
Electronic & Paper Claim Submission: Prepare and submit claims in a timely manner.
Copayment Collection: Ensure copays are collected; notify provider if payment method fails.
Payment Processing
Post payments and adjustments accurately while maintaining up-to-date patient account records.
Copayment & Payment Plans
Monitor copay collection, alert providers of failed payments, and assist patients with setting up and maintaining payment plans.
Accounts Receivable & Follow-Up
Conduct weekly aging reviews, follow up on outstanding claims (15–30+ days), and provide regular status updates.
Denials & Resubmissions
Investigate denied or rejected claims, correct errors, and resubmit with appropriate documentation to prevent recurrence.
Patient Support
Respond to patient billing inquiries with clarity and professionalism.
